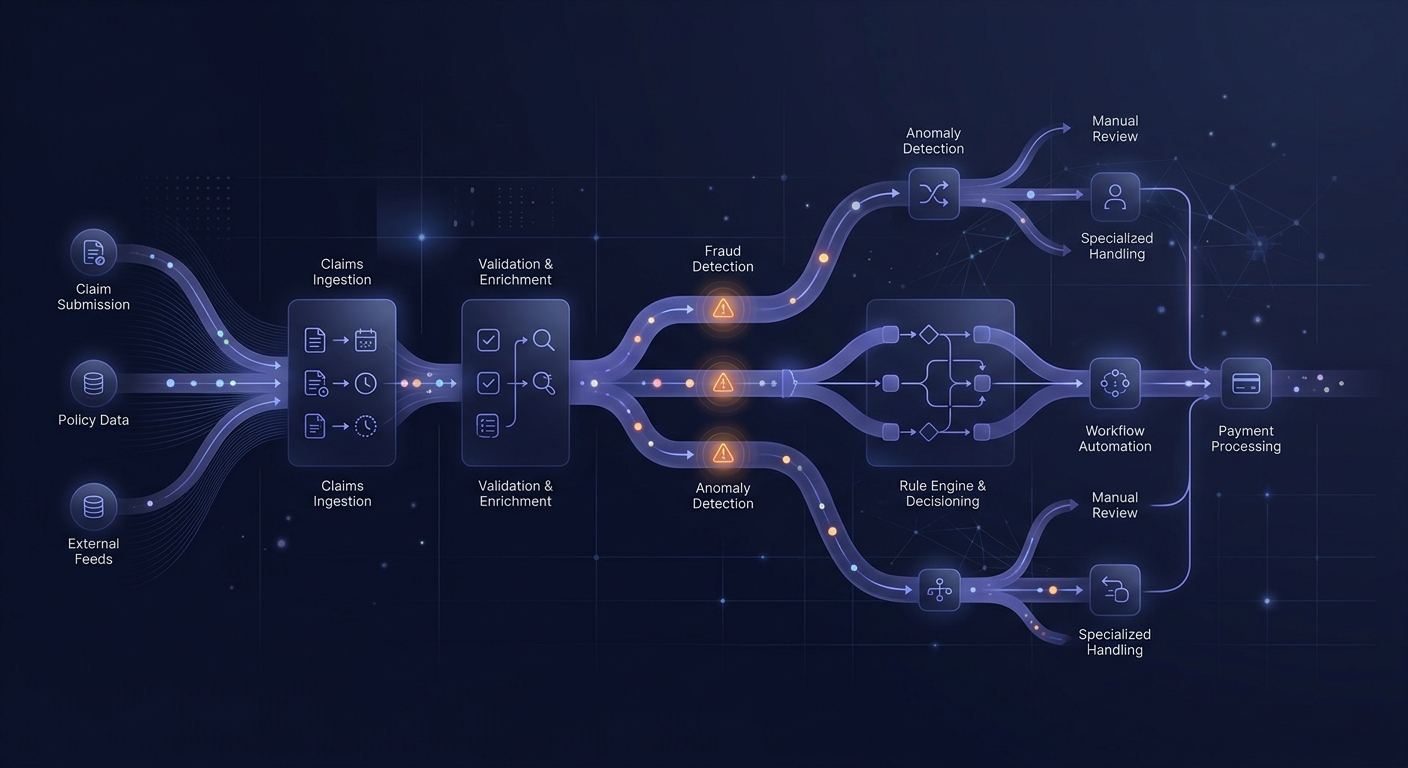
AI-Optimized PBM Claim Processing Pipeline
Pharmacy Benefit Management Organization
Overview
End-to-end modernization of a pharmacy benefit claims processing pipeline, replacing legacy batch workflows with an intelligent, event-driven system. The solution features AI-powered routing logic, automated anomaly detection, and configuration-driven adjudication rules that dramatically reduce manual intervention while improving accuracy and throughput.
Client Profile
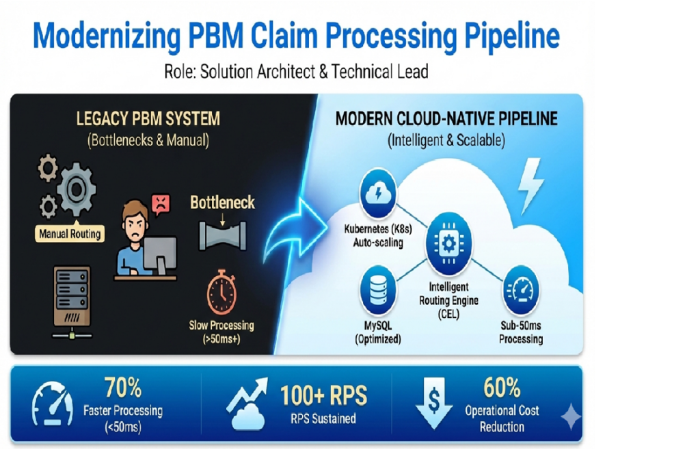
The Challenge
Scalability issues during peak processing periods
Lack of flexibility in routing claims to different adjudication platforms
Significant manual intervention requirements with no AI-driven decision support
Inconsistent processing times
Inability to handle peak loads during high-volume periods
Solution Architecture
Intelligent Routing Engine: Configuration-driven routing system directing claims to appropriate adjudication platforms. Implemented using Common Expression Language (CEL) for lightning-fast claim evaluation with zero-downtime configuration updates. AI models analyze historical claim patterns to optimize routing decisions.
High-Performance Backend: Built with Python for rapid development, leveraging async processing patterns and integrated CEL engine for complex rule evaluation.
Cloud-Native Infrastructure: Deployed on Kubernetes (K8s) with horizontal pod autoscaling, Application Load Balancer for traffic distribution, and MySQL database optimized for high-concurrency transactional workloads.
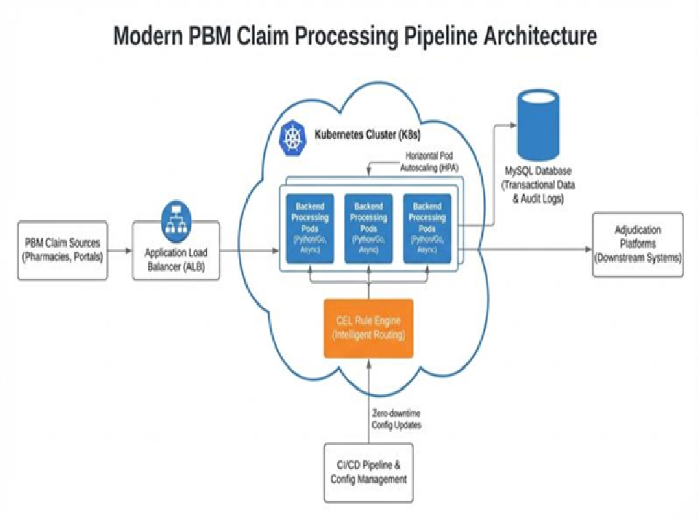
Architecture Diagram — AI-Optimized PBM Claim Processing Pipeline
Features & Capabilities
Sub-50ms Average Response Time
Consistent performance under high load with AI-optimized routing paths
Configurable Intelligent Routing
Dynamic, AI-informed decision-making based on business rules without code changes
Zero-Downtime Configuration Updates
Business teams modify routing logic in real time
Auto-Scaling Architecture
Kubernetes dynamically scales to handle 100+ requests/sec during peak traffic
AI-Powered Anomaly Detection
Automatic flagging of unusual claim patterns for review
Full Audit Trail & End-to-End Traceability
Every claim logged with timestamps, decisions, outcomes, trace IDs
High Availability & Fault Tolerance
Built-in retries, circuit breakers, and error handling
Rapid Platform Onboarding
New adjudication platforms integrated in days through configuration
Business Agility
Non-technical stakeholders manage routing policies via intuitive interfaces
Technology Stack
Security & Compliance
TLS 1.3 enforced at ALB, API layer, and database connections
MySQL encrypted with KMS; EBS volumes encrypted
IAM roles assigned to pods via Service Accounts; no static credentials
AWS Secrets Manager or Vault
Full audit log per claim with HIPAA retention; immutable storage in S3
Private subnets for pods and DB; security groups restrict access
HIPAA (with BAA), SOC 2 Type II, NIST SP 800-53
Results & Impact
Processing Time
0%
70% decrease in average claim processing time
Response Latency
Sub-50ms average per claim
Throughput
0+
100+ requests/sec sustained; 1M+ claims/month
Cost Savings
0%
60% reduction in operational overhead
Accuracy
0%
95% reduction in human error in claim direction
Platform Onboarding
New adjudication platforms integrated in days, not weeks
Deployment Frequency
0
2-4 deploys/week
Have a Similar Challenge?
We'd love to hear about your project and explore how we can help.