
RM Cobol to AI-Powered Cloud-Native: Modernizing Claims Processing
Mid-sized Healthcare Technology Company
Overview
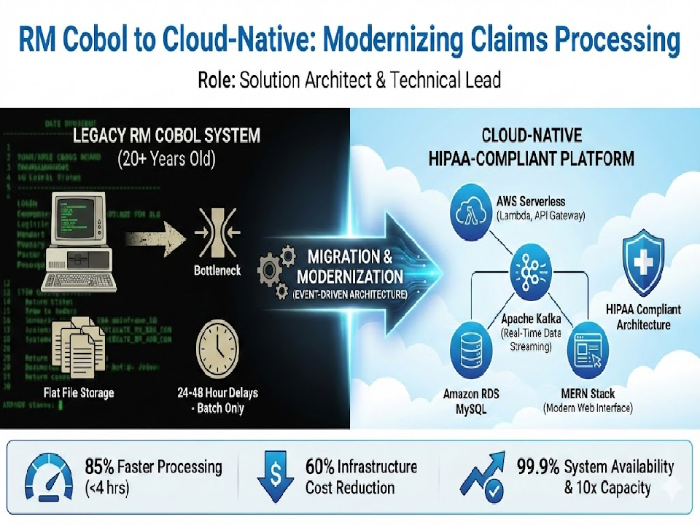
Complete transformation of a 20+ year-old RM Cobol claims processing system into a scalable, HIPAA-compliant cloud-native platform. The modernized solution leverages event-driven architecture, serverless computing, real-time data streaming, and AI-powered anomaly detection to deliver dramatic improvements in processing speed, reliability, and operational costs.
Client Profile
The Challenge
Batch-only processing causing 24-48 hour delays in claim adjudication
Flat file data storage severely limiting query, reporting, and AI-driven analytics capabilities
Rising maintenance costs with a shrinking pool of Cobol developers
No API layer, preventing integration with modern payer systems, clearinghouses, and AI services
Architecture gaps creating HIPAA compliance risks
Zero horizontal scalability during peak processing periods
Solution Architecture
Designed and implemented a modern, event-driven architecture replacing the monolithic Cobol system — with AI-assisted development pipelines accelerating the build and intelligent monitoring embedded throughout.
Data Layer Migration: Migrated from flat file storage to Amazon RDS MySQL with optimized schemas, proper indexing, and referential integrity. Implemented data validation rules previously embedded in Cobol business logic, enabling AI-powered anomaly detection on claims data.
Serverless Processing Engine: Built AWS Lambda functions for claim validation, adjudication rules, and batch processing. Integrated with API Gateway to expose RESTful endpoints for external system integration. AI-driven routing logic directs claims to the optimal processing path based on historical patterns.
Modern Web Interface: Developed a responsive MERN stack application (MongoDB, Express.js, React.js, Node.js) providing intuitive claim management, real-time dashboards, and AI-powered predictive reporting capabilities.
Integration Layer: Created secure API endpoints for third-party integrations including clearinghouses, payer systems, and healthcare information exchanges.
Event Streaming Platform: Deployed Apache Kafka as the central nervous system for real-time data synchronization. Implemented Change Data Capture (CDC) patterns enabling instant claim status updates across all downstream systems — feeding both operational dashboards and AI analytics models.
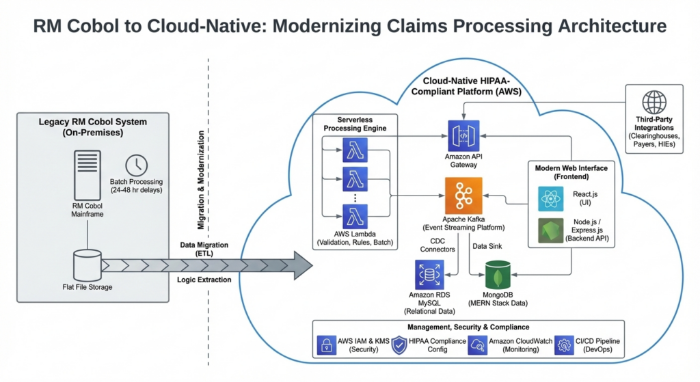
Architecture Diagram — RM Cobol to Cloud-Native: Modernizing Claims Processing
Features & Capabilities
Real-Time Claim Processing
Eliminated 24-48 hour delays; now under 4 hours from ingestion to adjudication with AI-assisted validation
Event-Driven Architecture
Apache Kafka as the central nervous system for instant data synchronization across systems
HIPAA-Compliant by Design
Full encryption (at rest & in transit), audit logging, RBAC, and secure PHI handling
Serverless Scalability
AWS Lambda auto-scales during peak loads without infrastructure management
AI-Powered Analytics
Real-time dashboards with predictive insights, anomaly detection on claims patterns, and automated trend analysis
Modern Web Interface
Responsive MERN stack app for claim tracking, dashboards, and reporting
Third-Party Integration Ready
RESTful APIs connect to clearinghouses, payers, HIEs, and EHRs
Automated CI/CD Pipeline
Blue-green deployments, rollback capability, IaC, automated testing with AI-assisted code review
Future-Proof Architecture
Modular design supports new features, AI models, partners, and compliance changes
Technology Stack
Security & Compliance
TLS 1.3 enforced at API Gateway, Kafka, and application layers
KMS-encrypted RDS, S3, and EBS volumes
IAM roles assigned to Lambda functions and services; least privilege principle applied; JWT-based authentication for web interface
All claim transactions logged with timestamps, user ID, IP, decision path, and outcome; immutable log storage in S3 with versioning + MFA delete
PII/PHI masked or excluded from UIs and logs; data minimization policy enforced
Private subnets for databases, Kafka, and Lambda; VPC endpoints for secure access
HIPAA (with BAA), SOC 2 Type II, NIST SP 800-53
Results & Impact
Claim Processing Time
0%
85% faster (from 24-48 hrs to under 4 hrs)
System Availability
0%
99.9% uptime achieved
Infrastructure Costs
0%
60% reduction in operational expenses
Concurrent Capacity
0x
10x increase in simultaneous users
Integration Capability
From 0 to 12+ connected systems
Compliance Status
Full HIPAA compliance achieved
Deployment Frequency
0
3-5 deploys/week (per module)
Latency
<0
<4 hours from claim ingestion to adjudication
Have a Similar Challenge?
We'd love to hear about your project and explore how we can help.